 
WHO Classifications of pulmonary hypertension This patient likely has acute worsening of her chronic pressures secondary to her severe acute pulmonary disease (PNA vs ARDS vs Pulmonary edema). Given pt’s history of autoimmune hepatitis, you and Cardiology suspect pulmonary HTN, specifically portopulmonary HTN (WHO Class 1). Now you are thinking something is straining your patient’s right heart, but you know from the RHC it’s not the left side of the heart so it has to be somewhere in between…the LUNGS! Cardiology consulted for RHC which showed severe pulmonary hypertension and elevated right sided filling pressures (RVSP at 70 mmHg). Severely elevated pulmonary artery systolic pressure. 
Worsening cardiomegaly when compared to prior CT this admission. Repeat CTA PE protocol returns negative for PE and shows resolving RUL infiltrate but worsening b/l groundglass opacities. Pt is stabilized and you obtained CT PE protocol and ECHO ICU course… Pt appeared fluid overloaded and placed on lasix drip. Some ST/Twave changes in the anterior leadsĭDx: Consider PE, ARDS, pna, ILD, valve rupture, intracardiac shunt, pHTN You see sinus tachycardia, rate around 100. She is tachycardic but with regular rhythm. Transmitted upper airway noises on auscultation but you hear b/l rales and rhonchi R>L. Tachypnic with shallow breathing on CPAP. Denies cough, CP, fevers, chills, AP, abdominal distention, n, v. Meds: lactulose, rifaximin, coreg for HTN. Unknown family history, former 5 pack years smoker. She completed 7 days of appropriate abx, and received IVF boluses. You send your intern to evaluate while you chart review to find out:Ħ3yoF PMH of HTN, autoimmune hepatitis c/b cirrhosis w/ esophageal varices s/p TIPS, admitted 7 days ago for sepsis 2/2 RUL pna. All rights reserved.You are on ICU and called to the floor for respiratory distress, respiratory rate 50s, despite being on CPAP. Approximately one-quarter of patients will have a new sinus tachycardia, and approximately one-quarter will have no change in their ECG.ĮCG changes with pulmonary embolism electrocardiographic changes electrocardiographic changes with pulmonary embolism pulmonary embolism.Ĭopyright © 2016 Elsevier Inc. The most common ECG changes when compared with previous ECG in the setting of PE are T wave inversion and flattening, most commonly in the inferior leads, and occurring in approximately one-third of cases. In 24.1% of patients, no new ECG changes were noted, with this finding more likely to occur in patients younger than 60 years. A new sinus tachycardia occurred in 27.3% of cases. 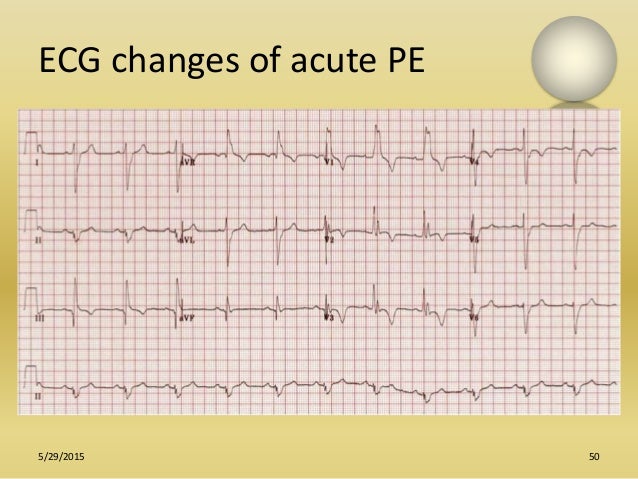
New T wave flattening, also most commonly in the inferior leads, was the second most common change, occurring in 29.5%. New T wave inversions, commonly in the inferior leads, were the most common change found, occurring in 34.4% of cases. Each patient's presenting ECG was compared with their most recent ECG obtained before diagnosis of PE.Ī total of 352 cases were reviewed. 
Our aim was to identify the most common ECG changes in patients with known PE when their ECGs were compared with their previous ECGs.Ī retrospective chart review of patients diagnosed with PE in the emergency department was performed. Previous studies have evaluated ECG patterns predictive of pulmonary embolism (PE) at the time of PE diagnosis, though none have examined ECG changes in these patients when compared with their previous ECGs. The electronic medical record is a relatively new technology that allows quick review of patients' previous medical records, including previous electrocardiograms (ECGs). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
